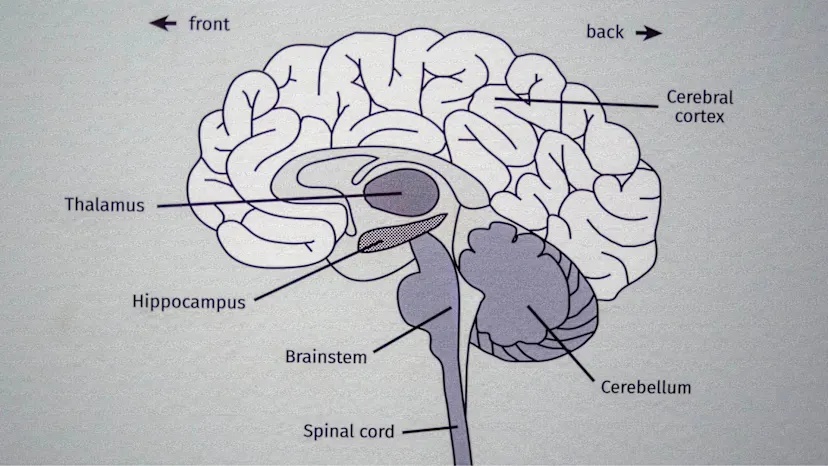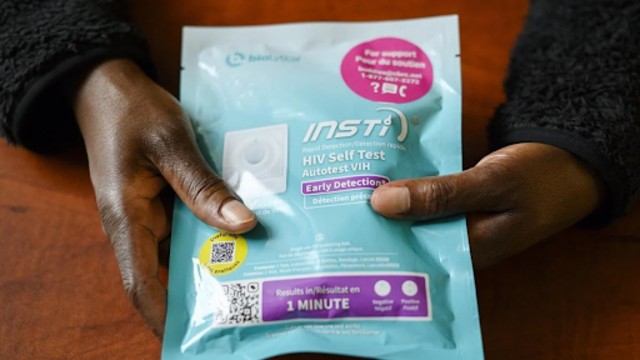
Prossy Luzige, a prevention and linkage coordinator who works in the York Region of Ontario, poses for a photograph with HIV self-test kits, photographed at the Toronto People With Aids Foundation office, in Toronto, Friday, Feb., 16, 2024.
Canada’s leading HIV experts have issued fresh guidance urging health-care providers to make preventive HIV medication far more accessible — and to stop “gatekeeping” treatment that could curb rising infections.
A national team of physicians has released a detailed clinical guideline designed to expand the use of antiretroviral drugs that help prevent HIV before and after exposure. The updated recommendations come as public health officials warn that Canada is off track to meet its 2030 goal of eliminating HIV as a public health threat.
The new guideline appears in the Canadian Medical Association Journal and reflects three years of research and review by 19 volunteer physicians.
Rising Infections Prompt Urgent Action
Canada recorded 1,826 new HIV diagnoses in 2024. Federal officials described this as a “small decline” after several years of steady increases. However, experts say the drop is too small to signal real progress, and several provinces continue to report rates well above the national average.
Manitoba and Saskatchewan remain hotspots, with infection levels three to four times higher than the country’s overall rate.
Health Minister Marjorie Michel noted that HIV continues to disproportionately affect people facing social and health inequities. This includes women, LGBTQ+ communities, people who inject drugs, and many Indigenous communities.
Who Is Most Affected?
The guideline highlights deep structural and historical inequities shaping Canada’s HIV landscape.
Women account for more than one-third of new infections. Gay, bisexual, and other men who have sex with men make up 38 per cent. People who inject drugs comprise another 25 per cent.
In some Indigenous communities — particularly across the Prairies — infection rates have reached alarming levels. Experts say these communities face heightened stigma, reduced access to health care, and limited public health outreach.
Dr. Darrell Tan, the guideline’s lead author, said it is “disappointing” that governments have not promoted PrEP and PEP with the same clarity they show for vaccines like the flu shot.
Ending Gatekeeping Around PrEP
The central message of the new guideline is clear: doctors should prescribe PrEP to anyone who asks for it, even if the person does not disclose their HIV risk factors.
Many people avoid sharing personal details due to stigma, shame, medical mistrust, or discrimination linked to racism, homophobia, transphobia, and colonial practices.
Removing these barriers, the authors say, is essential to reaching people who could benefit most.
Doctors from multiple fields — including primary care, reproductive health, and emergency medicine — are encouraged to actively offer PrEP when they identify risk behaviours such as condomless sex, prior sexually transmitted infections, multiple partners, or injection drug use.
More PrEP Options, Including Long-Acting Injectables
Since the last national guidance was released in 2017, PrEP options have expanded.
Along with daily pills and “on-demand” regimens, Health Canada approved a long-acting injectable medication in 2024.
The injection, administered every two months, may be particularly useful for people who struggle to take daily pills, including those experiencing homelessness or unstable living conditions.
Experts say this injectable form has “huge potential” to improve adherence and reduce infections.
Reaching Communities Most at Risk
Some researchers believe the guideline should have gone further in outlining strategies for high-risk regions — especially Prairie Indigenous communities, where HIV rates remain several times higher than the national average.
Advocates like Dr. Sean Rourke have been working directly with Indigenous leaders to fill that gap. A mobile HIV testing program launched in March has already tested more than 1,500 people in remote and underserved communities.
He says the tools to reduce infections already exist, but they require sustained support, outreach, and political will.
“It doesn’t happen on its own,” he said. “And that’s the problem.”